Key Takeaways
- Laparoscopic surgery offers faster recovery because it uses small incisions and causes minimal tissue trauma.
- Open surgery remains essential for complex, emergency, or large-mass cases requiring full visibility.
- Pain, infection risk, hospital stay, and wound complications are significantly lower with laparoscopic surgery.
- Most routine surgeries in 2026—hernia, appendix, gallbladder, uterus—prefer a laparoscopic approach.
- Surgeons decide based on safety, considering patient condition, disease severity, and anatomical factors.
- Laparoscopy improves mobility and reduces long-term risks such as incisional hernias and wound infections.
Introduction
Laparoscopic vs Open Surgery is one of the most researched surgical comparisons in 2026. Laparoscopic surgery generally offers faster recovery because it uses small incisions, causes less tissue trauma, reduces pain, and supports early mobility. Open surgery is still preferred for complex hernias, large tumors, emergency complications, and anatomical variations where direct access is essential.
When comparing Laparoscopic vs Open Surgery, patients want clarity on which option heals faster, is safer, and provides better long-term outcomes. Minimally invasive techniques have transformed surgical care in 2026, making laparoscopy the preferred approach for many abdominal and pelvic procedures. However, open surgery still plays a critical role in situations where minimal access is not safe or sufficient.
This guide provides an updated, evidence-based comparison to help you understand both approaches in detail.
What Is Laparoscopic Surgery?
Laparoscopic surgery, also called keyhole surgery, uses very small 0.5–1 cm incisions, a high-definition camera, and fine instruments to perform operations with minimal tissue disturbance. The surgeon views magnified images on a monitor, allowing precise movement without opening the entire abdominal wall.
Because the abdominal muscles remain largely intact, patients heal faster, experience less pain, and mobilize quicker compared to open surgery.
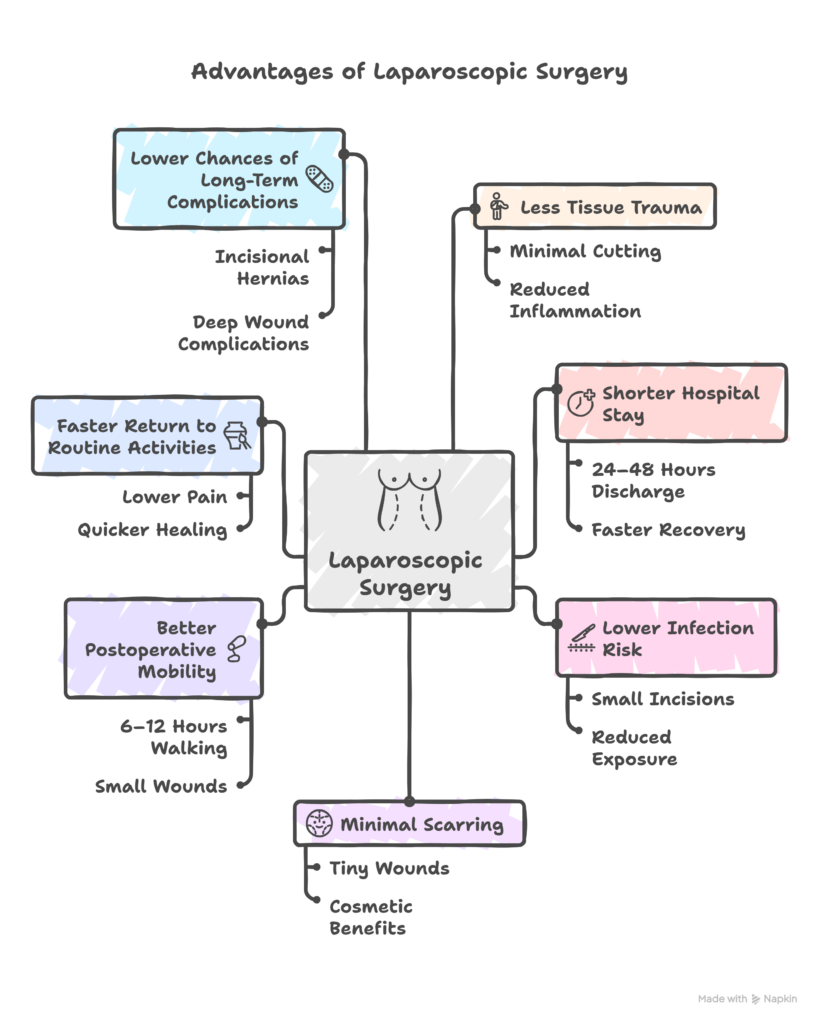
Benefits of the laparoscopic approach
1. Less Tissue Trauma
Minimal cutting and exposure reduce inflammation, leading to quicker healing.
2. Shorter Hospital Stay
Most patients are discharged within 24–48 hours due to faster postoperative recovery.
3. Lower Infection Risk
Small incisions reduce wound exposure, lowering infection rates significantly.
4. Minimal Scarring
Tiny wounds lead to excellent cosmetic outcomes, especially for younger patients.
5. Better Postoperative Mobility
Patients can usually walk within 6–12 hours because the wounds are small.
6. Faster Return to Routine Activities
Lower pain and quicker healing allow resumption of daily life much sooner.
7. Lower Chances of Long-Term Complications
The risk of incisional hernias or deep wound complications is significantly reduced.
What Is Open Surgery?
Open surgery is the traditional method where a large incision (6–12 cm or more) is made to provide direct access to organs. This approach remains crucial for complex cases, tumors, emergencies, or situations where minimal access is not safe.
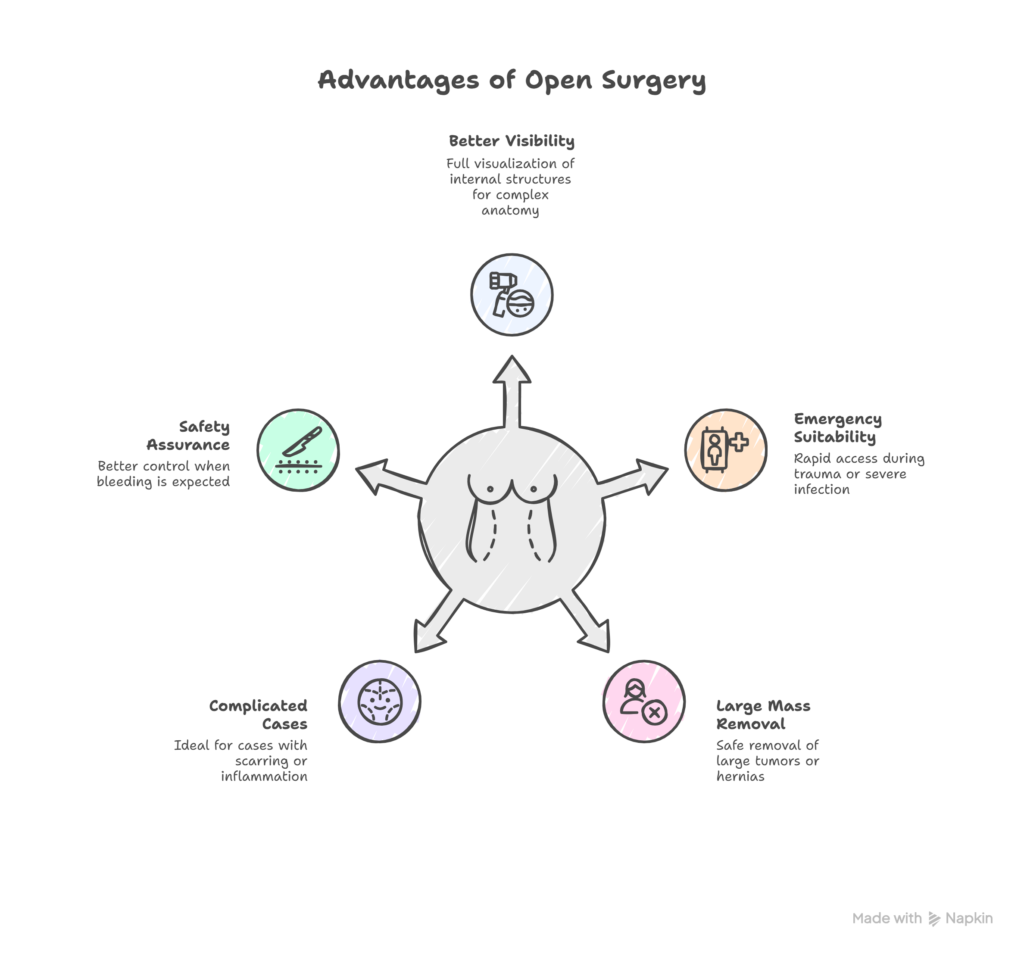
Advantages of Open Surgery
1. Better Visibility
A wide incision allows full visualization of internal structures, helpful in difficult anatomy.
2. Emergency Suitability
Open surgery ensures rapid access during trauma, perforation, or severe infection.
3. Able to Remove Large Masses
Large tumors or hernias often require full access for safe removal.
4. Ideal for Complicated or Recurrent Cases
Cases with heavy scarring or severe inflammation may not be suitable for laparoscopy.
5. Preferred When Safety Requires Full Access
If bleeding is expected or anatomy is unclear, open surgery provides better control.
Laparoscopic vs Open Surgery – Key Differences
Factor | Laparoscopic Surgery | Open Surgery |
Incision Size | 0.5–1 cm | 6–12 cm |
Pain Level | Low–Moderate | Moderate–Severe |
Recovery Time | 5–10 days | 2–4 weeks |
Hospital Stay | 24–48 hours | 3–5 days |
Blood Loss | Minimal | Higher |
Infection Risk | Low | Higher |
Cosmetic Result | Minimal scars | Visible scars |
Laparoscopic vs Open Surgery – Recovery Timeline
Laparoscopic Surgery Recovery
- Walking: Begins within 6–12 hours.
- Hospital stay: Usually 1–2 days.
- Daily activities: Restarted within 3–5 days.
- Return to work: Typically 5–10 days.
- Full recovery: Around 2–4 weeks.
Open Surgery Recovery
- Walking: Usually after 24–48 hours.
- Hospital stay: About 3–5 days.
- Daily activities: Restart after 1–2 weeks.
- Return to work: Often 2–4 weeks.
- Full recovery: About 6–8 weeks.
Benefits of Laparoscopic Surgery vs Open Surgery
1.Faster Recovery
Small incisions reduce trauma, enabling quicker healing and early mobility.
2. Less Pain and Discomfort
Minimal cutting of muscles leads to reduced postoperative pain levels.
3. Minimal Scarring
Cosmetically superior, as the scars fade to nearly invisible over time.
4. Lower Infection Risk
Small wounds result in fewer bacterial entry points.
5. Early Mobility
Patients typically stand and walk on the same day.
6. Lower Long-Term Complications
Reduced risk of incisional hernias and wound breakdown.
When Open Surgery Is Better in 2026?
1.Large or Complex Hernias
Strangulated or giant hernias often require open repair for better reinforcement.
2. Large Tumors or Masses
Bulky specimens cannot be removed safely through small port incisions.
3. Severe Infections or Emergencies
Open surgery allows rapid and direct access in life-threatening situations.
4. Multiple Previous Surgeries
Scar tissue from earlier operations may make laparoscopy unsafe.
5. Anatomical Variations
When organs deviate from typical positions, open access ensures safety.
Procedure-Wise Comparison (Hernia, Appendix, Uterus, Fibroids, Colon)
Laparoscopic vs Open Surgery for Hernia Repair
- Laparoscopic: Ideal for bilateral and recurrent hernias.
- Open: Required for strangulated or very large hernias.
Laparoscopic vs Open Surgery for Appendix
- Laparoscopic: Faster healing with less pain and scarring.
- Open: Preferred for perforated appendix or abscess cases.
Laparoscopic vs Open Surgery for Uterus Removal
- Laparoscopic: Best for standard hysterectomy with quicker recovery.
- Open: Required when fibroids are large or anatomy is complex.
Laparoscopic vs Open Surgery for Fibroids
- Laparoscopic: Effective for moderate-sized fibroids.
- Open: Needed when fibroids are too large or numerous.
Laparoscopic vs Open Surgery for Colon Procedures
- Laparoscopic: Standard for most colorectal diseases.
- Open: Needed in advanced cancer or emergency perforation.
Laparoscopy vs Robotic vs Laser Surgery
- Laparoscopy: Standard for most abdominal procedures due to its speed, safety, and minimal scarring.
- Robotic Surgery: Uses robotic arms for enhanced precision; best for pelvic and prostate surgeries.
- Laser Surgery: Best for piles, fissure, fistula, and varicose veins; not a substitute for abdominal laparoscopy.
Risk & Safety Comparison
Laparoscopic Surgery Risks
- Minor Risk of Organ Injury: Rare but possible with instrument introduction.
- Temporary Gas-Related Pain: CO₂ discomfort resolves within 1–2 days.
- Conversion to Open Surgery: Needed if visibility or bleeding becomes an issue.
- Small Risk of Port-Site Hernia: Significantly lower than open incisions.
- Anesthesia-Related Side Effects: Modern methods keep risks minimal
Open Surgery Risks
- Higher Infection Rates: Larger wound surface increases exposure.
- More Postoperative Pain: Bigger incisions cause more tissue disruption.
- Slower Recovery: Healing takes longer due to muscle splitting.
- Higher Incisional Hernia Risk: Large wounds weaken abdominal walls.
- Longer Hospital Stay: Needs extended monitoring and wound care.
- Higher Infection Rates: Larger wound surface increases exposure.
Surgeon’s Decision Checklist
- Age and Fitness: Determines tolerance to surgical stress.
- Comorbidities: Conditions like diabetes or heart disease influence healing.
- BMI: High BMI may impact laparoscopic visibility.
- Previous Surgeries: Scar tissue may require open surgery.
- Recovery Expectations: Patient goals matter in selecting the best approach.
- Size of Hernia/Tumor: Larger issues may need open surgery.
- Presence of Infection: Severe cases require full access.
- Urgency: Emergencies often need open intervention.
- Anatomical Variations: Altered anatomy may not suit minimal access.
- Bleeding Risk: Some cases require the control open surgery provides.
- Equipment Availability: Advanced tools are essential for laparoscopy.
- Surgeon Experience: Skill level determines safe technique selection.
- Emergency vs Elective: Emergencies may not allow time for laparoscopy setup.
- OT Infrastructure: Certain hospitals may limit laparoscopic options.
- Postoperative Support: Fast-track recovery pathways benefit laparoscopy.
Future of Minimally Invasive Surgery
- Micro-laparoscopy reduces incision size even further.
- Robotic platforms enhance precision in complex surgeries.
- AI-assisted imaging improves real-time decision making.
- Same-day discharge becomes more common post-laparoscopy.
- Overall complication rates continue to decrease with new technology.
Laparoscopic vs Open Surgery — Which Is Better?
When comparing Laparoscopic vs Open Surgery, most patients benefit more from the laparoscopic approach because it involves smaller incisions, less pain, and a faster recovery. Open surgery is still important for complex or emergency cases where broader access is required, but for routine abdominal procedures, laparoscopy is generally safer, quicker, and more comfortable.
Ultimately, the best choice depends on your condition, medical history, and the surgeon’s expertise.
Dr. Varun Kumar J, an experienced Laparoscopic, Laser & General Surgeon, evaluates each case individually to recommend the safest and most effective approach. With advanced training in minimally invasive techniques, he helps patients achieve faster recovery and better surgical outcomes.

About the Surgeon
Dr. Varun Kumar J is a highly experienced Laparoscopic, Laser & General Surgeon practicing in Bangalore and Mysore. He specializes in minimally invasive procedures for hernia, gallbladder disease, appendicitis, colorectal conditions, and anorectal disorders. With thousands of successful surgeries and a focus on enhanced recovery, he emphasizes safety, precision, and faster patient outcomes.

